- THE PITT: 10 MEDICAL DETAILS THE SHOW GETS WRONG, AND 10 DETAILS THEY GET RIGHT - 2 Apr 2026
- ANESTHESIOLOGY AND MALPRACTICE LAW - 23 Mar 2026
- PHYSICIAN ASSISTED SUICIDE IN THE USA AND SWITZERLAND - 12 Feb 2026

What were the ten most significant advances in anesthesiology in the past decade, 2010 – 2020? Here are my picks:

- Sugammadex. Sugammadex was FDA-approved in December 2015, and the practice of chemically paralyzing surgical patients and reversing their paralysis has been forever changed. For my non-medical readers, sugammadex is an intravenous drug which reverses the paralysis of rocuronium, the most commonly used anesthetic paralytic drug, in approximately one minute. Sugammadex replaced the decades-old practice of injecting a combination of neostigmine and glycopyrrolate to reverse paralysis. Neostigmine and glycopyrrolate were slow to act (a wait of up to nine minutes), and could not reverse paralysis if zero twitches were present on a nerve stimulator monitor. In addition, 16 mg/kg of sugammadex IV can reverse an intubating dose of rocuronium, which makes rocuronium more quickly reversible than succinylcholine for rapid sequence intubation. Sugammadex is not cheap (a cost of $100 per 200 mg vial), but since the availability of sugammadex, no anesthesia practitioner should ever have an awake and still-paralyzed patient at the conclusion of an anesthetic. A terrific advance. Five stars.

- Management of acutely ill COVID patients. In a demanding short time frame, anesthesiologists and other critical care physicians developed safe measures to intubate COVID patients and to manage their failing organ systems during intensive care unit admissions. Because every severely ill COVID patient eventually wound up on a ventilator, the role of anesthesiologists to safely place endotracheal tubes and help manage respiratory failure in the ICU setting was invaluable. In addition, the American Society of Anesthesiologist’s support of the standard that every elective surgical patient must have a COVID test done preoperatively has been vital. The medical literature supports the fact that COVID patients have increased complications after anesthesia and surgery. An asymptomatic COVID-infected patient should never have elective surgery.

- Use of Zoom. In the era of COVID, Zoom videoconferencing made person-to-person communication involving anesthesiologists possible. During the early days of the COVID outbreak, the American Society of Anesthesiologists was able to keep its members informed and educated via Zoom conferencing. At the present time, almost all anesthesia continuing medical education (CME) is conducted effectively via Zoom. I attend the Stanford anesthesia Grand Rounds each Monday morning via Zoom, and the educational value is as high as it was when I attended in person. Expect Zoom CME to continue as a major vector in the years to come. Although Zoom may adversely affect in-person attendance at medical meetings forever, I believe widespread videoconferencing education is a tremendous advance. Five stars.
- The Stanford Anesthesia Emergency Manual. See this link. The algorithms set out in the red laminated ring-bound Stanford Anesthesia Emergency Manual filled a fundamental need in acute care medicine. When perioperative emergencies arise, a delay in treatment can result in death or irreversible brain damage. The presence of this Stanford book of checklists assures that every operating room is equipped with the cognitive aids needed for standard of care treatment. The manual is available at https://emergencymanual.stanford.edu. The authors chose not to glean profits from the publication of the Stanford Emergency Manual, but instead made it available for physicians and nurses everywhere for free. Five stars.

- Safer care. Anesthesia care has become safer and safer. Deaths and adverse outcomes continue to decrease because of improved monitoring, vigilance, education, and training. The Cleveland Clinic writes, “In the 1960s and 1970s, it wasn’t uncommon to have a death related to anesthesia in every one of every 10,000 or 20,000 patients. Now it’s more like one in every 200,000 patients—it’s very rare.” The continuing advances in anesthesia safety are a bellwether for other specialties, who must envy the progress made in anesthesiology quality assurance. The Anesthesia Patient Safety Foundation is a hub of all advances. Five stars.


- Pubmed/Internet/the Cloud. This past decade saw an explosion of handheld mobile devices and phones, as well as an expansion in the use of the cloud and the internet. Anesthesiology benefited from these technological advances. Information regarding anesthesia care is immediately available to any anesthesia provider anywhere in the world, if they have internet access. The ability to do a Google search on any topic is outstanding and immediate. Pubmed is a National Library of Medicine website which catalogs an abstract on every medical publication. Pubmed is an essential tool for every physician who is investigating previously published medical knowledge. Five stars.
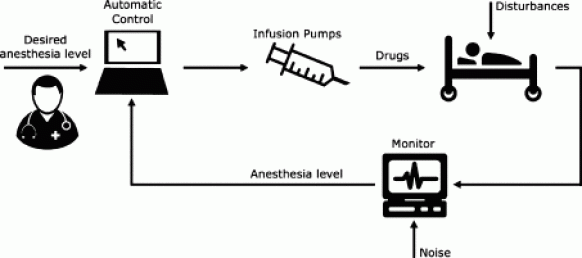
- Closed loop TIVA (total intravenous anesthesia). Anesthesiologists and pharmacologists have been working on the pharmacokinetics of automated administration of intravenous anesthetics for years. Utilizing EEG monitoring data (BIS monitor levels) to titrate the depth of anesthesia shows promise. For a typical anesthetic, TIVA requires more work than vapor anesthesia with sevoflurane, because the anesthesiologist must load a syringe with propofol and/or remifentanil, attach an infusion line, load the syringe into the infusion pump, and program the pump to the correct infusion rate. In contrast, a sevoflurane vaporizer is already loaded with liquid anesthetic, is easy to use, and merely requires the pushing of one button and turning of one dial. Closed loop TIVA is not in clinical use at this time, but you can expect that the future, anesthesia recipes will include automated sedation/anesthetic depth titration via computer administration. The TIVA research of the past ten years has paved the way for this advance. Three stars.

The ultrasound-guided regional anesthesia boom. In the past ten years the number of ultrasound guided regional anesthesia blocks has mushroomed. Regional nerve blocks decrease the need for postoperative narcotics. Evidence shows that ultrasound guidance reduces the incidence of vascular injury, local anesthetic systemic toxicity, pneumothorax and phrenic nerve block for interscalene blocks, but there has not been consistent evidence that ultrasound guidance is associated with a reduced incidence of nerve injury. The ultrasound-guided regional anesthesia boom has led to tens of thousands of additional nerve blocks, and an unfortunate fact is that a small but non-zero number of these patients develop permanent nerve damage in their arms or legs after their blocks. Regional anesthesia specialists who publish in the medical literature have made little effort to quantify or report these complications. Prospective data on nerve injuries is needed. Honest verbal informed consent to each patient before a nerve block is needed. See this link. Three stars.

Point of care ultrasound (POCUS). In recent years, anesthesiologists began to aim their ultrasound probes at the abdomen, thorax, and airway, to gain real-time information and immediate knowledge of the anatomy and pathology beneath the skin and to better manage and treat critically ill patients. POCUS is proving useful in trauma , chest examination, and pediatric anesthesia. Because POCUS is a recent development, the majority of anesthesiologists do not have the training, skills, or knowledge needed to use this new technique. Recent graduates of residency and fellowship programs will lead the way as the anesthesia workforce transitions toward mastery of POCUS. Three stars.

- ASA Monitor/Dr. Steven Shafer. I list this development last, but my enthusiasm for the ASA Monitor and its Editor-in-Chief Steven Shafer is extremely high. The American Society of Anesthesiologists revamped their ASA Monitor publication into a monthly newsletter reporting up-to-date information regarding our specialty. The ASA hired Steven Shafer MD PhD as the editor. Dr. Shafer is a Professor of Anesthesiology at Stanford, and is an outstanding scientist, author, and humorist. I’ve known Steve for nearly forty years, since he was a medical student. He has authored more than 200 peer-reviewed publications in the field of anesthesiology, and was the Editor-in-Chief for Anesthesia and Analgesia from 2006-2016. Dr. Shafer possesses a razor-sharp intellect and a flippant sense of humor seldom seen in scientific writing. His lead editorial in each month’s issue of the ASA Monitor is required reading for every anesthesia professional. Dr. Shafer also personally authors a daily update on COVID research and statistics—a Google group which you can personally subscribe to as an email offering. See this link. Five stars.
*
*
*
The most popular posts for laypeople on The Anesthesia Consultant include:
How Long Will It Take To Wake Up From General Anesthesia?
Why Did Take Me So Long To Wake From General Anesthesia?
Will I Have a Breathing Tube During Anesthesia?
What Are the Common Anesthesia Medications?
How Safe is Anesthesia in the 21st Century?
Will I Be Nauseated After General Anesthesia?
What Are the Anesthesia Risks For Children?
The most popular posts for anesthesia professionals on The Anesthesia Consultant include:
10 Trends for the Future of Anesthesia
Should You Cancel Anesthesia for a Potassium Level of 3.6?
12 Important Things to Know as You Near the End of Your Anesthesia Training
Should You Cancel Surgery For a Blood Pressure = 178/108?
Advice For Passing the Anesthesia Oral Board Exams
What Personal Characteristics are Necessary to Become a Successful Anesthesiologist?
READ ABOUT RICK NOVAK’S FICTION WRITING AT RICK NOVAK.COM.


One thought on “THE TEN MOST SIGNIFICANT ADVANCES IN ANESTHESIOLOGY IN THE PAST DECADE”