- AI IN MEDICINE –IT’S IN YOUR POCKET - 30 Apr 2026
- THE PITT: 10 MEDICAL DETAILS THE SHOW GETS WRONG, AND 10 DETAILS THEY GET RIGHT - 2 Apr 2026
- ANESTHESIOLOGY AND MALPRACTICE LAW - 23 Mar 2026

You’re the anesthesiologist on call on a Saturday night. A patient arrives at the Emergency Room complaining that he ate piece of steak one hour ago, and the meat got stuck in his throat. He is morbidly obese patient who stands six feet tall and weighs 350 pounds, for a BMI of 47.
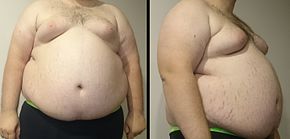
The attending general surgeon wants to do an upper GI endoscopy to extract the piece of meat from the patient’s esophagus or push it through into the stomach. He’s called on you to do the anesthetic.
What do you do?
You examine the patient and find he has a short neck, a small mouth, and a large tongue. You cannot see his soft palate at all, and you rate him as a Mallampati 4.

The patient is alert, and is an excellent historian. He cannot even swallow his saliva. He has no difficulty breathing or significant chest pain. His hospital chart shows no past anesthetics, and he has no medical problems except hypertension which is treated with lisinopril. His vital signs are normal, and his oxygen saturation is 96% on room air.You are six months out of anesthesia training and new to this hospital. The surgeon—a 60-year-old male with the brash confidence of General Patton—is an iconic and respected figure at this medical center. He wants to proceed at once. It’s 8 pm on a Saturday night. He requests “just a little sedation” so he can insert the endoscope past the gag reflex and into the esophagus.
You bring the patient into the endoscopy suite, attach the standard vital signs monitors, and administer oxygen via a Procedural Oxygen Mask (POM, made by Mercury Medical).

You administer 2 mg of Versed and 100 micrograms of fentanyl IV. The surgeon sprays Cetacaine into the patient’s mouth for topical anesthesia and inserts a bite block. After five minutes time the patient is still wide awake. The surgeon looks at you and says, “I need him a little deeper than this.” You administer another 1 mg of Versed and 50 micrograms of fentanyl. After another five minutes time, the patient is still wide awake. The surgeon looks at you and repeats, “I need him a little deeper than this.” He says this in an impatient condescending tone, and you feel pressured. You administer 50 mg of propofol, and the patient’s eyes begin to drift closed. The surgeon inserts the gastroscope, after which the patient coughs, gags, and vomits into his airway. His oxygen saturation which had been 100% quickly plummets to 75%. You move to the head of the bed, suction the patient’s mouth, and attempt bag-mask ventilation without success. His oxygen saturation drops to 60%. You reach for a Miller 3 laryngoscope and attempt to intubate the trachea, but you cannot visualize his vocal cords. You are panicked. The surgeon is screaming at you to do something. You tell the surgeon he needs to do a tracheostomy. In the meantime you insert a laryngeal mask airway into the patient’s throat, but are still unable to ventilate the lungs. The ECG rhythm converts to ventricular fibrillation, and you call a Code Blue.

After thirty minutes of CPR and ACLS, the patient is declared dead.
What went wrong here? A patient who walked into the hospital is now dead. The basic problem was that the anesthesiologist proceeded to deeply sedate a patient with a full stomach (a known aspiration risk) without first controlling the airway by inserting an endotracheal tube. This morbidly obese patient with a thick neck, a small mouth, and a large tongue was always going to be difficult to intubate, but a successful intubation was most likely to occur under controlled circumstances with the patient awake prior to any endoscopy. The issue of a domineering surgeon pushing an inexperienced anesthesia provider into doing the wrong anesthetic is a key problem. This can and does happen, and once the case has concluded with a bad outcome, that same surgeon will deny any culpability, step back and say “I don’t do anesthesia. The decisions and actions of the anesthesiologist caused the problem, not me.”
How should the anesthetic have been done?

In a parallel universe, an experienced anesthesiologist would do the following:
- Explain to the surgeon and the patient that the meat stuck in the esophagus presents a dire risk of aspiration into the lungs and loss of airway, and explain to them that the case must be done either entirely awake without sedation (unlikely to be successful), or as a general anesthetic with an endotracheal tube placed prior to any endoscopy intervention.
- This case is best done in an operating room, rather than in an endoscopy suite.
- The anesthesiologist will assemble all emergency airway equipment, including a Glidescope, a fiberoptic laryngoscope, the entire difficult airway cart, and the scalpel, bougie, tube equipment for an emergency cricothyrotomy.
- The anesthesiologist will likely call in a second pair of experienced hands, either a second anesthesiologist or perhaps the in-house emergency room physician most experienced with intubating patients.
- A rapid sequence intubation with propofol, succinylcholine, and cricoid pressure is a possible approach, but runs the risk that if the airway is so difficult that the endotracheal tube cannot be passed on the first attempt, the patient will be difficult to ventilate, difficult to oxygenate, and the meat and saliva from the esophagus could aspirate into the airway, leading to a hypoxic emergency.

- A safer approach is an awake oral intubation using a fiberoptic laryngoscope. The back of the operating room table is inclined upward into a sitting position. Topical anesthesia and local nerve blocks of the airway are performed. See the footnote below (referenced from Miller’s Anesthesia) for a detailed description of the airway anesthesia.A Moderate sedation with Versed and fentanyl is administered, but the patient is kept awake. There’s still a risk that the topical anesthesia will blunt the cough reflex if the patient regurgitates the meat, so suction and a MaGill forceps are immediately available.

- The anesthesiologist inserts the fiberoptic scope through an endotracheal tube (ET tube) and advances the scope into the mouth until he or she is able to visualize the vocal cords. This can be difficult and may take time, but there is no acute emergency, so an unhurried approach is warranted. Once the fiberoptic scope is threaded through the vocal cords, the patient will most likely cough violently and will require some restraint by two individuals, one on each side of the bed. The ET tube is threaded over the scope quickly and the balloon on the ET tube is inflated. The tube is connected to the anesthesia machine circuit and end-tidal CO2 is confirmed. At this point an IV bolus of propofol and rocuronium is administered to induce general anesthesia.
- Once the ET tube is taped securely in place, the surgeon can position the patient as he desires for the upper GI endoscopy. Anesthesia is maintained with sevoflurane and oxygen. When the surgeon is finished, the patient is awakened using sugammadex as necessary to reverse the muscle relaxation. When the patient opens his eyes, he can be safely extubated.
What are the lessons to be learned from this case study?
- Don’t be intimidated or pushed into an unsafe anesthesia plan. Do what you were trained to do in residency, and stick to safe anesthesia practice. If an adverse outcome occurs, claiming the surgeon made you do something unsafe will not help you one bit. You are in charge of all anesthesia decisions.
- In anesthesia practice and all acute medicine care, you must manage Airway-Breathing-Circulation (A-B-C) in that order. Anesthesiologists are trained as airway experts, and for this reason we are the most vital acute care physicians in a medical emergency. The airway must managed first.
- Take great care when anesthetizing a morbidly obese patient. They are at higher risk for anesthetic complications. They are also at greater risk for surgical and perioperative medical problems. See the lay press coverage in U.S. News and World Report, and also another post from this blog.
- Maintain your skills in awake intubation. No anesthesiologist uses awake intubation often. For nearly every patient the appropriate sequence is to induce anesthesia first and intubate the trachea afterwards. But some patients: e.g. those with ankylosing spondylitis, congenital airway deformities like Treacher Collins syndrome, or certain patients with morbidly obesity or super morbidly obesity (BMI > 50), awake intubation is indicated. One of my professional partners, a former Senior Examiner for the American Board of Anesthesiologists, told me that during national anesthesia oral board examinations, when a patient presented with severe airway abnormalities for a surgical case, it was very common for successful examinees to state they would perform an awake intubation. Why? Because an awake intubation burns no bridges. The patient is unharmed by general anesthesia until the ET tube is already in place, and thus is unlikely to have a Cannot Intubate-Cannot Ventilate situation that can lead to life-threatening hypoxia. And as well, in an oral exam the examinee doesn’t have to actually perform the procedure—they only have to state they could do it successfully.
- How do you maintain your skill in awake intubation? This is the tough question. When I was in residency training, Dr. Phil Larson, a former Chairman of Anesthesia at Stanford and former Editor-in-Chief of the journal Anesthesiology, taught us elective awake intubation on patients with normal airways, who did not require an awake intubation, so we could hone the skill. Each patient was sedated with IV narcotics. Local lidocaine nerve blocks were done, and an injection of local anesthetic was administered through the cricothyroid membrane, all prior to us performing the awake fiberoptic intubation successfully. Did this take extra time? It did. The intubation and anesthesia induction took ten minutes instead of one minute. Did the surgeons mind? They didn’t, because they respected Dr. Larson, they were glad an excellent anesthesiologist was attending to their cases, and they realized that nine minutes of time was no big deal. Am I recommending you do this in your practice? No, but in this age of the Glidescope, many anesthesiologists have forgotten how to utilize a fiberoptic intubation. I recommend you practice fiberoptic intubation on asleep patients, and maintain the skill.
You may need it to save someone’s life one day.
Footnote:
A. (From Chapter 44, Airway Management in Adults, Miller’s Anesthesia, Ninth edition, pp 1373-1412) “Topical application of local anesthetic to the airway should, in most cases, be the primary anesthetic for awake airway management. Lidocaine is the most commonly used local anesthetic for awake airway management because of its rapid onset, high therapeutic index, and availability in a wide variety of preparations and concentrations. Benzocaine and Cetacaine (a topical application spray containing benzocaine, tetracaine, and butamben; Cetylite Industries, Pennsauken, NJ) provide excellent topical anesthesia of the airway, but their use is limited by the risk of methemoglobinemia, which can occur with as little as 1 to 2 seconds of spraying. . . . A mixture of lidocaine 3% and phenylephrine 0.25%, which can be made by combining lidocaine 4% and phenylephrine 1% in a 3:1 ratio, has similar anesthetic and vasoconstrictive properties as topical cocaine and can be used as a substitute. Topical application of local anesthetic should primarily be focused on the base of the tongue (pressure receptors here act as the afferent component of the gag reflex), the oropharynx, the hypopharynx, and the laryngeal structures; anesthesia of the oral cavity is unnecessary. . . . Before topical application of local anesthetic to the airway, administration of an anticholinergic agent should be considered to aid in the drying of secretions, which helps improve both the effectiveness of the topical local anesthetic and visualization during laryngoscopy. Glycopyrrolate is usually preferred because it has less vagolytic effects than atropine at doses that inhibit secretions and does not cross the blood-brain barrier. It should be administered as early as possible to maximize its effectiveness. “. . . Oropharyngeal anesthesia can be achieved by the direct application of local anesthetic or by the use of an atomizer or nebulizer. Topical application of local anesthetic to the larynx can be achieved by directed atomization of a local anesthetic or by the spray-as-you-go (SAYGO) method, which involves intermittently injecting local anesthetic through the suction port or working channel of a flexible intubation scope (FIS) or optical stylet, as it is advanced toward the trachea.“Topical application of local anesthetic to the airway mucosa using one or more of these methods is often sufficient. If supplemental anesthesia is required, then a variety of nerve blocks may be used. Three of the most useful are the glossopharyngeal nerve block, superior laryngeal nerve block, and translaryngeal block. The glossopharyngeal nerve supplies sensory innervation to the posterior third of the tongue, vallecula, the anterior surface of the epiglottis, and the posterior and lateral walls of the pharynx, and is the afferent pathway of the gag reflex. To block this nerve, the tongue is displaced medially, forming a gutter (glossogingival groove). A 25-gauge spinal needle is inserted at the base of the anterior tonsillar pillar, just lateral to the base of the tongue, to a depth of 0.5 cm. After negative aspiration for blood or air, 2 mL of 2% lidocaine is injected. The process is then repeated on the contralateral side. The same procedure can be performed noninvasively with cotton-tipped swabs soaked in 4% lidocaine; the swabs are held in place for 5 minutes.”
*
*
popular posts for laypeople on The Anesthesia Consultant include:
How Long Will It Take To Wake Up From General Anesthesia?
Why Did Take Me So Long To Wake From General Anesthesia?
Will I Have a Breathing Tube During Anesthesia?
What Are the Common Anesthesia Medications?
How Safe is Anesthesia in the 21st Century?
Will I Be Nauseated After General Anesthesia?
What Are the Anesthesia Risks For Children?
The most popular posts for anesthesia professionals on The Anesthesia Consultant include:
10 Trends for the Future of Anesthesia
Should You Cancel Anesthesia for a Potassium Level of 3.6?
12 Important Things to Know as You Near the End of Your Anesthesia Training
Should You Cancel Surgery For a Blood Pressure = 170/99?
Advice For Passing the Anesthesia Oral Board Exams
What Personal Characteristics are Necessary to Become a Successful Anesthesiologist?
READ ABOUT RICK NOVAK’S FICTION WRITING AT RICK NOVAK.COM.

